Thursday, December 23, 2010
Being Motivated "Towards"
I think it is interesting that motivation towards something is more effective at generating action than motivation away from something. I used to clean my house to get away from messiness, I now clean it to move towards control, order, and a more peaceful atmosphere. Towards motivation does seem to be more effective in this particular instance.
Felice's post focuses on motivation for choices while preparing for childbirth. Fear of pain (an away from motivation) is a common motivation for women in this situation,. Early on in my first pregnancy, when I was planning on getting an epidural, I was motivated by fear of pain. When I discovered the risks of epidurals, I was still motivated by fear--fear of complications resulting from overuse of medical interventions. This is still an away from motivation, even though it was movtivating me in a completely different direction--to have an unmedicated birth. I started to discover other motivations in that pregnancy, but did not have a lot of time to explore them.
In my second pregnancy, I was not so afraid of intervention. I'd had a medically managed birth that turned out fine. I had some fears, but they were more fears of "failing" (in quotes, because I now realize that the word failure has no place in birth) than of complications. I was determined that (of course as long as there were no complications) I was going to do it without drugs. I was motivated to prove that I could do it. I was motivated away from failing. I was also motivated towards an enjoyable birth, a safe birth, an empowered birth--and I worked to keep my choices in line with what these words meant to me at the time, which I'm sure was very different from what they would have meant early in my first pregnancy. They probably mean something slightly different even now.
When we move away from being motivated away from pain and away from "failure" and learn to be motivated towards the most positive safe birth experience we can have, it is then that we discover that gettting a "perfect" birth experience doesn't matter so much and are able to embrace whatever birth gives us and learn and grow from it.
Thursday, December 9, 2010
Doula mini-documentary
Monday, December 6, 2010
The Myth of "Early Labor"
As a science, medicine seeks to define things in specific terms. As a natural process, childbirth doesn't always fit into perfect little boxes. Childbirth education often uses the explanations from medicine in attempts to help women understand the birth process. However, based on my own observations, the "textbook labor" does not apply to the experiences of a very large proportion of birthing women, and I wonder if we are, by using it, doing women a disservice by creating false expectations.
The general model that is taught is that there are three stages of birth: dilation, pushing, and birth of the placenta. Within the dilation stage, three phases are taught: the early/latent phase, active phase, and "transition."
- Early phase is usually defined the time when the cervix is going from 0-3 cm dilation, and is characterized by pressure waves that are spaced far apart and my be irregular.
- Active phase is defined as cervical dilation from about 4-7 cm, and is when the waves get regular and increase in intensity and frequency and cause measurable cervical change.
- "Transition" is when the cervix goes from 8-10 cm, and is usually explained by its physical and emotional intensity and the presence of symptoms such as shaking, nausea, and vomiting.
- If this is the "normal" birthing women whose births do not fit this pattern may consider what they experience as "abnormal."
- It relies very heavily on measuring the cervix as a basis for knowing how far along a woman is.
- Some women's cervices will be reach dilations where thy should be in "active phase" but stay there for days or weeks before the baby is born, and there is nothing pathological going on
- I specifically disagree with the way "early/latent phase" is characterized.
I have been participating in an online support forum for women who are planning natural births for about 3 years now. On our group, we have a fun tradition called Lodges, which are a sort of journal for pregnant women that lasts from 36 weeks to about 1 month postpartum. I have followed many lodges in the past three years, so I have read updates from women as they are nearing the births of their babies. From my own informal observations, it appears to me that a majority of women experience periods of regular and intense pressure waves (not Braxton Hicks, but the same kind you have during birthing) on and off for days, weeks, and in some cases months, before giving birth. They will go long periods with no pressure waves, then have them start again for a few hours, then they'll go away. So, does early labor stop? Can early labor last for two weeks? Or is our idea of "early labor" a myth?
Some people would call the off-and on periods of pressure waves "false labor," but I really dislike that language because it implies that the woman doesn't know what she's feeling. In many cases, the only way to tell the difference is in retrospect: sometimes they go away and sometimes they continue to the birth of a baby, they usually don't really feel much different from each other, contrary to what some will tell you. "False labor" also implies that it is not doing anything, and I am of the opinion all pressure waves do something, even if it is not causing measurable dilation. It could be effacing the cervix or encouraging the baby to rotate into a better position. In some cases, dilation is occurring, just not quickly enough for it to be measurable. For women who have "false labor," it may just be that their body does the "early labor" work incrementally, with long periods of rest.
The problem is that I suspect that the majority of women don't know how common start-stop labor (as I like to call it) really is. I recently read a blog post by a nurse (shared on facebook by The Deranged Housewife) who blamed the "need" for hospitals to use pitocin on women going to the hosptial and getting epidurals too early. Comments on the facebook link suggested that the problem is not the patients themselves, but that someone is failing to adequately inform them what the end of pregnancy is really like. The nurse's post really made me wonder how many women are getting pitocin for "stalled labor" when actually they were having an episode of pressure waves that would have gone away? How many of these babies would actually have come days or weeks later without the pitocin?
(On a similar note, I also love this post by midwife Stephanie of Vita Mutari questioning the logic that it is "safe" to "labor at home as long as possible" in order to avoid crowding the labor and delivery floor and avoid interventions, yet "unsafe" to plan a homebirth with a midwife.)
The concept of "early labor" is misleading because it is so easy to mistake start-stop labor for "early labor," and if women assume "this is it"and run to the hospital at the first sign of a pressure wave, they are guaranteed to either be sent home disappointed or have a whole lot of interventions, and neither of those is a desirable thing. I know I fell into the "early labor" trap myself with my first birth--I remember thinking "I've been in early labor for two days and I'm only 1 centimeter?"
For real, human women, not mythical "textbook" ones, the onset of the birthing time is a fluid process that they may move in and out of at their own unique pace. The last few weeks of pregnancy are the orchestra tuning up before the concerto, the engines revving before the race.
Tuesday, November 30, 2010
Order in Our Lives, Even with a Baby
I recently realized that I my kids and I really needed a little more order and structure in our lives. I realized that I felt overwhelmed by my house never being clean, and I was using the computer as an escape from my responsibilities. When I did clean, I would exhaust myself trying to clean everything at once, and then I would feel "burned out" from cleaning and wouldn't maintain it, and the house would soon deteriorate into chaos again. I really wanted to develop the concept of rhythm for my kids, as taught in Waldorf education (which I have been studying after Sheridan blogged about the changes she is making in her home now that her kids are going to a Waldorf-inspired charter school), but I realized it wasn't possible with the level of chaos in our environment.
I found a wonderful system for establishing habits of cleanliness. It's Flylady's Beginner Babysteps. I am on Day 8 today, which means I have been doing it for a week, and the improvement is slow, but it is lasting change, not a temporary fix. I feel like I am finally getting some control in my life. One of the routines is you get dressed first thing in the morning, from head to toe. This encouraged me to finally go out and get my hair cut. I hadn't had my hair cut since I was pregnant with my son, who is almost 9 months old. And my kitchen is clean, which means I can actually cook dinner for my family.
I have been limiting my computer time, and as a result haven't been working on blog posts as much. I have a second post in the works about the book I read, Sisters on Journey, which I will hopefully finish eventually. If you don't hear from me, I am probably either enjoying my kids or working on creating a more peaceful environment for them.
Tuesday, November 23, 2010
A Birthy Thanksgiving
In my First Pregnancy and Birth:
- I'm grateful that I found information about natural childbirth. The paradigm shift I experienced changed me forever, and having had both a pro-epidural and low intervention attitude, I understand better where people are coming from.
- I'm grateful that I asked questions of the OB I had been seeing and realized his policies were not good obstetric medicine so that I didn't end up giving birth with him as my provider.
- I'm grateful that I found a wonderful midwife group who took me at 34 weeks and were very supportive and made me feel comfortable.
- I'm grateful that I learned how harmful going to the hospital too early can be.
- I'm grateful that I experienced pitocin induction, so I can sympathize with other women who have had it.
- I'm grateful that I had an epidural, both because it was what I needed at the time and because it taught me to be able to tell other women that sometimes the epidural is the best choice for that particular birth.
- I'm grateful that my epidural worked as it should, not too numb and not ineffective, and my baby was born without needing any further intervention.
- I'm grateful that I tore so I can empathize with women recovering with perineal stitches.
- I'm grateful that my husband was exactly what I needed him to be through the whole experience.
- I'm grateful that my birth experience was not exactly what I wanted because it inspired me to prepare more for my second birth and was part of what inspired me to pursue a career as a birth professional.
- I'm grateful for my beautiful, healthy little girl, who is now almost three.
- I'm grateful that I ended up with an amazing OB, who restored my faith in the profession.
- I'm grateful that I experienced the benefits of using Hypnobabies during my pregnancy
- I'm grateful that I can compare pitocin induction to spontaneous labor.
- I'm grateful that I got to labor as long as I did in the comfort of my own home.
- I'm grateful that I learned that I had the power to make my birth much more comfortable with focus and relaxation.
- I'm grateful that I progressed smoothly and arrived at the hospital at 8 cm, which further removed the temptation of pain relief.
- I'm grateful that I didn't know I was GBS positive so I didn't go to the hospital earlier, and that my baby was still healthy.
- I'm grateful that I learned how hard it can be to maintain focus with hospital distractions.
- I'm grateful that I wasn't able to keep using my Hypnobabies during second stage so I can understand how intense natural childbirth can be.
- I'm grateful that I did not tear and got to experience how much smoother recovery goes with an intact perineum.
- I'm grateful that my nurse carefully read my birth plan.
- I'm grateful that my husband exceeded my expectations as a birth partner.
- I'm grateful that my mother-in-law did not circumcise my husband, so my husband and I easily agreed to leave our son intact.
- I'm grateful that my experience with this birth reinforced my interest in becoming a Hypnobabies Instructor.
- I'm grateful for my beautiful, healthy 8 month old boy, who thinks he is a toddler already.
Happy Thanksgiving, everyone!
Monday, November 22, 2010
Traditional Birth Secrets: The Rebozo
A rebozo (pronounciation) is a woven piece of fabric used by Mexican women as a shawl, a baby carrier (similar to the way I use a wrap, but the fabric is not as long), and a comfort and positioning tool for pregnancy and childbirth.
Courtesy of Special Collections, University of Houston Libraries
Techniques for the Rebozo in childbirth include:
- "sifting" the mother
- to aid in the double hip squeeze
- rocking or dangling the mother
- covering the mother's eyes and ears to block distractions
- for the mother to pull on, especially during pushing
Here is the above technique being used in at the hospital during a pitocin induction:
The technique used in the above two videos are explained more in-depth at the Spinning Babies website.
In my doula training, I learned how to do a technique called a "double hip squeeze" with my hands to open the pelvis. This video explains how to use the Rebozo to make the double hip squeeze easier:
More articles and pictures:
- The Rebozo: a transcript of a rebozo workshop given by Doña Irene Sotelo and Naolí Vinaver, published in Midwifery Today (more pictures can be seen by following the link below the photo shown)
- "Comfort Measures for Childbirth: Let's do it with a Rebozo"--a collection of images by Patti Ramos taken at a rebozo workshop with Guadalupe Trueba, including images of the rebozo used for rocking , putting it over the eyes to block out distractions, to pull on while pushing, and other uses
- The Many Uses of a Rebozo at Birthing Essentials--short explanations with pictures of many of the techniques
Saturday, November 20, 2010
Research-backed Benefits of Hypnosis for Childbirth
- 51% less likely to use drugs for pain relief (38% of the hypnosis group used pain medications, compared to 74% in the control group)
- 70% less likely to have their labors augmented (11% in the hypnosis group were augmented, compared to 70% in the control group)
- 67% more likely to have a spontaneous vaginal delivery (meaning they were not induced and did not have cesareans)
Despite it being a meta-analysis, the sample sizes are still quite small. As far as I can tell, the control group represents the standard population, which would include women who do not do any childbirth preparation and/or who planned to have epidurals. It would be interesting to see research comparing women using hypnosis with other methods of natural childbirth preparation, since that would provide a clearer picture of the unique benefits of hypnosis.
One reason why hypnosis is such an effective method of birth preparation: research shows women are more easily hypnotized during pregnancy.
Wednesday, November 17, 2010
Joseph B. DeLee: Obstetrics that Sucks
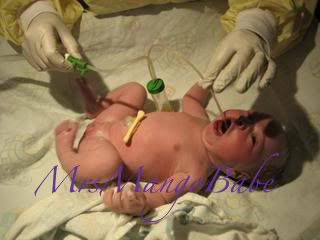
My first baby being suctioned with a DeLee Mucus Trap
Joseph B. DeLee, inventor of the suctioning device still commonly used in American hospitals today (though routine suctioning might actually be harmful), was an obstetrician in the early 1900s. In my Childbirth International workbook, I came across this lovely quote from him:
Obstetrics has a great pathologic dignity. Even natural deliveries damage both mothers and babies, often and much. If childbearing is destructive, it is pathogenic, and it if is pathogenic it is pathologic
If the profession would realize that parturition viewed with modern eyes is no longer a normal function, but has imposing pathologic dignity, the midwife would be impossible even of mention.-Dr. Joseph DeLee, 1915
Sometimes the words of Dr. DeLee are so extreme they sound like satire. They're not. The guy was serious. I first read about him in Tina Cassidy's book Birth, the Surprising History of How We are Born, which is a very easy-to-read tracing of the history of obstetrics and midwifery in the U.S.--The author of which, who had a standard hospital birth-turned-cesarean for her first birth, came out of the writing of the book a believer in midwifery, and had a HBAC with her second child (you can find the story if you dig around the archives of her blog). It was also in Cassidy's book that I first learned that a large percentage of women in the late 19th and early 20th century, including the population DeLee would have treated, were afflicted with rickets, a bone softening disorder caused by Vitamin D deficiency that often caused people to have severely deformed pelvises.With a quick googling his name, I found that Jill at the Unnecessarian has already posted a whole series on the writings of Joseph B. DeLee:
- Joseph Bolivar DeLee and the Prophylactic Forceps Operation
- Joseph DeLee's 1915 Campaign to Eliminate the Midwife
- Joseph DeLee Warns Colleagues in 1940 About "Streamlined Labors"
Obstetricians, as members of society, tend to blind faith in technology and the mantra: technology = progress = modern. The other side of the coin is the lack of faith in nature, best expressed by a Canadian obstetrician: 'Nature is a bad obstetrician.' So the idea is to conquer nature and results in the widespread application of attempts to improve on nature before scientific evaluation. This has led to a series of failed attempts in the twentieth century to improve on biological and social evolution. Doctors replaced midwives for low risk births, then science proved midwives safer. Hospital replaced home for low risk birth, then science proved home as safe with far less unnecessary intervention. Hospital staff replaced family as birth support, then science proved birth safer if family present. Lithotomy replaced vertical birth positions, then science proved vertical positions safer. Newborn examinations away from mothers in the first 20 minutes replaced leaving babies with mothers, then science proved the necessity for maternal attachment during this time. Man-made milk replaced woman-made milk, then science proved breast milk superior. The central nursery replaced the mother, then science proved rooming-in superior. The incubator replaced the mother's body for care of low-weight newborns, then science proved the kangaroo method better in many cases....Routine pitocin and cord traction replaced physiological delivery of the placenta, then science found a natural third stage superior for low risk women.
-Marsden Wagner, MD, MSPH, Fish Can't See Water: The Need to Humanize Birth in Australia
Science has helped American maternity care come a long way from DeLee's time, but the fact remains that the roots of our obstetric system are in the ideas of people who had a lot of things about birth wrong, at least when applied to a population of women with normally developed pelvises. I also believe he was wrong about midwives. Obstetrics (speaking of the profession generally and not of specific members) will continue to be at odds with those who support the midwifery model as long as it continues to dismiss the value of childbirth knowledge gathered by those who learn by being with woman.
Saturday, November 13, 2010
How you can win a Baby Bond--the nursing cover that covers you and not your baby
Sheridan at EnjoyBirth is giving away a sample Baby Bond Flex that she reviewed. Click here to learn how you can win!
Tuesday, November 9, 2010
Results Are In: Austrailan Study Supports Physiological Third Stage!
I just learned today (thanks to Birth Sense) that the Australian researches who wrote the theory paper have completed a study on third stage management. The abstract is available here, and the results are very interesting! The study found that for low risk women, active management in a hospital was actually associated with a significantly higher rate of postpartum hemorrhage (11.5%) than the rate they found for midwife-led "holistic physiological care" in a freestanding birth center (1.7%). Considering that previous studies had found the risk or hemorrhage using other definitions of "expectant management" to be higher, these findings are important for determining what factors are necessary for a safe, natural third stage.
Monday, November 8, 2010
Birth and Death: "to mourn with those that mourn"
I have been reading my second book for the Childbirth International book review assignment (the first one inspired me to write posts on progesterone and celebrating fertility). My local library had a book that was on the list called, Sisters on a Journey: Portraits of American Midwives by Penfield Chester. Chester interviewed 27 midwives for the book, and each chapter tells one of their stories, each in that midwife's own words. I am really enjoying reading all the different perspectives. I find it inspiring, for any future midwifery aspirations I may have, but also for doula work, as it has taught me that doula-ing is actually a very large part of midwifery.
One of the common themes in the interviews is dealing with the responsibility of life-or-death situations and the possibility of death being so close. Honestly, this is something that terrifies me about the idea of becoming a midwife. I don't want the pressure to have to make such important decisions and have to act quickly and skillfully in a crisis. This book has taught me that my feelings are normal and has helped me learn how midwives may deal with that responsibility. I also learned that birth and death have a lot in common. Here is one example that stood out to me, from the interview with renowned midwife, Ina May Gaskin.
In our community, although we had never read anything about this, it was the midwives that naturally gravitated toward being with families who were dealing with death. Everyone noticed that death felt much like birth, that there was the same sort of energy--a very heightened awareness. Things and people looked dear to you; you had the sense of life being precious, of the need to be good to each other, of the need to be thankful for life, of the need to be attentive to what you had to say, of the need to mix sadness and laughter, to tell stories, to come together and be very human with each other. Not to think about money, not to think about what would anybody think.That's all I am going to quote here, but Ina May also explained more about how midwives are like "gatekeepers" of birth and death, and also told the story of her daughter's death at a young age.
My own baby was the first one in our community that died. I was in the first few months of my midwifery practice, exhausted and anemic, and he was born very premature and lived for twelve hours. I knew that he couldn't have been saved a the time, so we didn't go to the hospital. We did what we could, but I knew from losing him, I learned a lot. I think if it had happened to somebody else I wouldn't be a midwife now. But because I had the support of the community, I learned about grieving. I also knew that in some what that happened to teach me something important as a midwife and so I tell that story. I've learned about healing, and I learned about how you treat somebody when they've lost a baby.
(Chester, Sisters on A Journey, 1997, pg. 132-133)
I recently saw the film The Curious Case of Benjamin Button, and though I found the film very long and the ending, sad, I learned the lesson I think it was trying to teach--growing up and getting old are really the same, just in opposite order, and life is really more of a circle than a line. Based on this perspective, birth and death are basically the same.
October 15th was Pregnancy and Infant Loss Remembrance Day. As I lit my candle that evening, I thought of my friend who lost her baby in her second trimester recently. I was very affected by the loss, since we had discussed her preparations for the birth and I had offered to serve as her doula. I found I needed to cry alone about it, and I don't think I would have anticipated that happening.
Last week I learned that my high school U.S. History A.P. teacher, now retired, was killed in a car accident while traveling in Greece. She was my favorite teacher, an entertaining storyteller whose love of history really shined in her teaching. She was an inspiration, the kind of educator I aspire to be. Any time such a vibrant person leaves this world, it kind of brings you face-to-face with your own mortality.
Through all of these experiences and learning, the following passage from the Book of Mormon has been on my mind:
...and now, as ye are desirous to come into the fold of God, and to be called his people, and are willing to bear one another’s burdens, that they may be light;These verses represent the covenant one makes when joining our faith. Interestingly, the last part of it is quoted in the document I wrote about in my Guest Post at the Gift of Giving Life. It is the part before that which I have been thinking about, especially "to mourn with those that mourn." If we have charity and love others as God loves them, we will have the desire to support others through their journeys in life. This includes things like crying with someone who is in the middle of grief. I have been thinking that maybe working with pregnant and birthing women, in the fragile time of newly developing life, who will sometimes not keep that life as long as we all would want them to, will be my personal way to fulfill my promise "to mourn with those that mourn."
Yea, and are willing to mourn with those that mourn; yea, and comfort those that stand in need of comfort, and to stand as witnesses of God at all times and in all things, and in all places...(Mosiah 18: 8-9)
Friday, October 29, 2010
Will We Ever Reach Peace in the OB v. NCB war?
I was recently surfing a blog called OB/Gyn Kenobi, because I thought the name was really clever, written by an anonymous obstetrician who calls herself Dr. Whoo? I haven't read a lot on her blog, but I can tell that she believes in individualized patient care and recognizes that the issue of liability in the American legal system is a huge problem for her profession. I came across one post where she expressed a lot of frustration about how the natural birth community views obstetricians, automatically assuming that they are all the same horrible stereotype. She points out that in her current practice, there is a split in philosophy between the older generation and her own younger generation.
My personal experiences corroborate her observations, as the OB I saw during my first pregnancy before switching to a midwife group, was an older doctor, and he had a "my way or the high way" attitude, complete with continuous EFM, mandatory IV infusion, NPO, and pushing on your back only. He believed that episiotomy is necessary for about a third to half of all women and that all women change their minds about wanting a natural birth when they are in labor. The OB/Gyn I saw in my second pregnancy was younger and was nothing like this--she was supportive of low-intervention birth if all was going well, and had attended many unmediated labors. She almost never did episiotomies, and actually encouraged me to write a birth plan.
It is wrong to define obstetrics by extreme negative examples. There are great OB/Gyns out there. I'd like to hope that there are a lot of them.
One of Dr. Whoo?'s most compelling points is this:
Perhaps the most disheartening thing, is that there can be no real dialogue between the two philosophies, so jaded are our particular perspectives.I appreciate that she acknowledges that the obstetric side has a jaded perspective, too. This is evidenced by some of the comments on the post:
The fan page looks good so far. You might want to include links to things like: Mothers in Medicine, pages where people can get real information about Ob/Gyn services (other than the doctor hating, "busness of being born" websites)Condescending, much? Here is another
go to alldoula.com I went there trying to figure out what a doula was. They are very anti-OB and also are giving very bad advice to pregnant women.That almost makes me ashamed to call myself a doula. And this one
Do any of these doctor bashing twits realize that just a few generations ago women DIED from "natural" at-home childbirth (the only kind going, back then) on a regular basis?I would be remiss if I didn't address the fallacy of the "women used to die and now they don't" argument. You can not compare statistics from different time periods and assume that one change in that time is the determining factor in the change in statistics. Natural birth advocates know that hosptials and interventions have benefits and save lives in certain situations. That is why women who plan to birth at home have a plan for transfer to the hospital if complications arise. The burden of reaching out the olive branch of peace is really on us because we need obstetricians. Modern homebirth, though significantly safer than homebirth in antiquity (due to sanitation and better midwifery knowledge and emergency medications that can be given in the home), can never really be safe without hospital back up. All too often, women who transfer to the hospital from a planned homebirth are met with hostility for choosing not to use the hospital and then needing it after all. The truth is she needed you all along, just in a different way than you wanted her to need you.
We need to focus on what we have in common--a desire to improve birth for everyone. We may have different opinions about how that can be done, but we will never get anywhere if we keep making this a war. Division is hurting us, and hurting mothers and babies. We cannot afford to alienate all of the the obstetricians our there who care deeply about mothers and babies and make birth their life's work! Just as there are various types of natural birth advocates, each obstetrician is an individual person. Many of these people are caring and sensitive and we push them away with our belief in an extreme stereotype. It is bigotry, and I am done with it. I am committing now to make my blog a doctor-friendly zone. I want better care for pregnant women and their babies and that is only going to come about with peace and collaboration.
Tuesday, October 26, 2010
check out Candy Clips by B for cute and simple hair accessories
Saturday, October 23, 2010
Elective Cesareans as Commentary on a Failed Birth Model
While I have strong opinions about what constitutes safe childbirth, I respect the rights of all women to make their own choices about their births. It appears that in reaction to the strong natural childbirth presence on the internet (where many women get support that they do not get from their doctors, families, or local girlfriends), there are now websites with the purpose of promoting elective cesareans as a viable birth choice.
Many birth advocates (perhaps myself not exempt) are guilty of using fear of cesareans as a springboard. I realize that most of the stuff out there is attempting to dissolve some of the fear that surrounds c-sections, and I don't really have a problem with that. I would prefer for women for whom the benefits of having a c-section clearly outweigh the risks to be able to go into their cesarean birth without fear. As I have said before, I am all for lessening fear in all types of birth. However, what good does it do to attempt to make vaginal birth sound scary in order to make c-sections sound less scary?
The September 2009 opinion piece at Pregnancy Zone, The Benefits of A Cesarean Section Delivery, which one of my friends at an online community recently shared, is one such attempt. The article was bombarded by comments from women who disagreed with the point of view of the author and criticized her approach of using generalized claims without evidence to support them. I think the two sides of this argument are starting out with different basic assumptions that prevent them from effectively communicating with each other.
The author of the article is assuming that the alternative to a cesarean section is the typical medical model hospital birth. On the other hand, most of her opponents are likely working from very different construct of "vaginal birth" (such lack of understanding is quite common in internet mommy wars). I'm not going to argue about whether the claims made in the piece are true, but rather to look at her characterization of vaginal birth and what that says about our maternity care model and birth culture.
In the "No Labor Pain" section she brings up three kinds of pain associated with vaginal birth: contractions, perineal stitches, and hemorrhoids. When discussing contractions, she assumes that all women see birth as a necessary evil to get over with in order to get a baby. She compares being in labor to recovering from surgery. She assumes that "most" women receive episiotomies (and don't have a choice in the matter) and seems to feel that stitches in the abdomen are preferable to stitches in the perineum. Even without episiotomy, there are a lot of women who assume tearing is inevitable. The author also assumes that hemorrhoids are common in vaginal birth. So, in this author's view, a woman who has a vaginal birth not only has "labor pain" but also a painful, messy recovery involving a sensitive area.
The "Dignity and Privacy" section assumes that all women giving birth are dehumanized and violated, mentioning the presence of a multitude of medical strangers doing vaginal exams and being in a "less than flattering position for any number of hours." At best, this birth sounds like pseudo-surgery, and at worst like sexual assault and torture. No wonder women want to be disconnected from this.
What does the fact that there are women who view vaginal hospital birth as less desirable than cesarean surgery say about how our system treats vaginal birth? Has our system really made birth so clinical, unknown, and scary that major abdominal surgery sounds preferable to a normal human process?
If birth is just a clinical baby extraction, it does make sense that women would prefer to do it through their bellies instead of their vaginas. But this doesn't make sense to women who see labor as a rite of passage, a challenge to rise to, or even a joyful experience that doesn't have to be painful. Natural birth advocates know that with the right kind of care, vaginal birth with an intact perineum or with very minimal tearing is very possible and that vaginal birth doesn't have to permanently damage the vagina. For women who understand humanized birth, it is sad to realize that women think vaginal birth has to be demeaning and rape-like. With sensitive, respectful care, when women choose their own labor positions and choose when they have vaginal exams (or not to have them at all), vaginal birth can be dignified, private, and even empowering.
Perhaps the question physicians should be asking themselves is not, Should we perform cesareans at a womans's request? but, What have we done to vaginal birth to cause women to request cesareans?
Wednesday, October 20, 2010
Great Minds Think Alike
Christa's birth is unlike any other hospital birth I've seen. She was not hooked up to a single machine, there were no wire or cords or tubes attached to her, she wore her own robe (the hospital gown was behind an armchair - lol - I'm assuming it slipped off the back of the chair), she snacked on crackers and sipped Gatorade, Norah Jones was playing on the iTunes, and I'm honestly surprised she gave birth on the bed :) Christa didn't spend much time on the bed until right when the baby was born.The images are stunning and it's really special to see such a home-like birth in a hospital setting captured in photos. Jessica and I thought it was interesting that we both came up with the same phrase to describe low-intervention birth.
Monday, October 18, 2010
Hands-off Neonatal Care
Suctioning of newborns is very common in U.S. hospitals. MidwifeThinking has an excellent post on meconium that also details the risks of routine suctioning. I actually did not know that routine suctioning was not done in other developed countries, so I found it enlightening to hear the perspective of a UK-trained midwife practicing in Australia on this.
I have discussed the theory that immediate skin-to-skin after birth may reduce the risk of postpartum hemorrhage. It also influences the initiation of breastfeeding. This video (which I saw for the first time when Bonnie shared it on her blog, Birth-Joy) demonstrates the results of a study that found that not only was a baby's ability to self-initiate breastfeeding affected by pain medication used in labor, but also by whether or not the mother and baby were separated following the birth.
Given the benefits of skin-to-skin contact, I feel that hospitals really should work to make initial skin-to-skin between mother and baby possible. Here is an excerpt from what I hope will be a great tool for improving hospitals in this reguard. (Thanks to Rixa, who posted this after seeing a presentation on it at the Lamaze/ICEA MegaConference)
Friday, October 15, 2010
Pregnancy and Infant Loss Remembrance Day

Please visit www.october15th.com to learn more about Pregnancy and Infant Loss Remembrance Day.
For all who have lost babies, born or unborn, my heart goes out to you and my thoughts are with you today. No one may know why your child could not be with you longer. All life is fragile, but it seems it is often even more so when it is brand new. As someone who has chosen to pursue a career in birth, I know this is something I have to live with, but I am still learning how.
Tuesday, October 12, 2010
Discovering and Celebrating Female Fertility
When one of my peers asked about it in the class about puberty at school, we were told that the non-blood secretions from the vagina were "bacterial discharge"--sounds nasty. How I wish we could have been taught by someone who knew the truth--that the white/clear stuff is actually a fluid produced by the cervix in response to normal hormonal changes during the cycle. Of course, going into specifics about how observing it for pregnancy achievement or birth control would not be appropriate for this age group, but now seeing the ignorance of those who were supposed to be teaching us about our bodies, I can't help but feel a bit betrayed.
For some great suggestions and links about celebrating your daughters becoming women, see The Menarche at Bellies and Babies.
I also wanted to share a few links for some great online resources about fertility charting:
The Beautiful Cervix Project offers some cool pictures to supplement study of Fertility Awareness. It started with a woman using FAM for birth control sharing the photos she took of her cervix each day of her cycle, documenting the changes in it along with the other fertility signs she charted. The site has now expanded to include many different types of cervix pictures.
And here are a few sites that currently offer free charting software:
Saturday, October 9, 2010
Progesterone: the pro-gestation hormone
Progesterone's Role in the Menstrual Cycle
This chart shows the changes in hormone levels throughout the female cycle.
 (image originally uploaded to Wikimedia by Shazz)
(image originally uploaded to Wikimedia by Shazz)- Follicle Stimulating Hormone
- Estrogen
- Luteinizing Hormone
- Progesterone
Progesterone has a warming effect on the body, which is why there is a shift in basal body temperature after ovulation. Progesterone sustains the lining of the uterus for the second half of the menstrual cycle, until the corpus luteum disintegrates, resulting in a drop in progesterone, which triggers menstruation. In late 2006 and early 2007, after I went off the birth control pill, before my daughter was conceived, I was anovulatory. My gynecologist prescribed an oral form of progesterone, which I was to take for a few days and then the drop in progesterone would trigger a bleed, which it did.
If the corpus luteum is not producing enough progesterone, the uterine lining would be unable to support implantation of a fertilized egg, often characterized by either spotting in this phase or menstruation starting too soon. In the fall of 2008, when I was breastfeeding my daughter, I was having issues with constant spotting. I took an herb called Vitex, which is said to increase the progesterone secreted by the corpus luteum. The spotting stopped, and I began to have menstrual cycles, so whatever the Vitex did to my hormonal balance, it worked.
Progesterone's Role In Pregnancy
If the egg is fertilized and implants, it secretes HCG, which is the hormone that changes the color of the second line on the pregnancy test. HCG tells the corpus luteum not to disintegrate and it continues to secrete progesterone, keeping the contents of the uterus in, until the placenta is fully formed and takes over the secretion of this hormone. The warming effect of progesterone continues in pregnancy, so the woman's core temperature remains at the slightly elevated post-ovulation level.
Initiation of labor is a complex process, and what exactly starts it is not known. A signal from the fetal lungs is proven to be one factor. Progesterone withdrawal, like that which causes menstruation, is a well-known theory, and probably also plays a role. Progesterone is said to inhibit oxytocin. That would explain why most women do not experience pre-term labor from activities that increase oxytocin levels, such as sex or breastfeeding. Oxytocin is free to cause contractions after the progesterone level has dropped.
While I was looking for links for my resource list on indications for induction, I found a Cochrane Review on the use of progesterone supplementation to prevent pre-term birth in at-risk women. The review found the progesterone made a significant difference in the women who carried their babies to term. Perhaps the placenta not producing enough progesterone is one cause of pre-term labor, just like not enough progesterone in early pregnancy is one cause of miscarriage. Just as it did during the luteal phase, progesterone keeps the contents of the uterus in.
Perhaps lowered progesterone levels when spontaneous labor is imminent is the reason that natural and low-tech induction methods such as membrane stripping (which triggers prostoglandins), breast pumps (which trigger oxytocin), and intercourse (which, if done correctly, does both), only start labor "when the body is ready." You can also see how trying to use artificial oxytocin to induce women whose progesterone level is still high could be tricky.
The body's process of starting labor and the role of different factors in it is something I'm quite curious about and hope more research is done on in the future. I'd be very interested to know what causes contractions to change from Braxton Hick's to ones that feel more intense, and why some women experience these more intense contractions on and off for days or weeks before entering active labor.
The more I learn, the more amazed I am by the human female body!
Tuesday, October 5, 2010
I babywear
 My son likes to snuggle in my homemade cotton jersey no-sew wrap (instructions here). It makes it easier for him to block out distractions and fall asleep, and then I can put the edge of the cloth over his head so it stays secure while he sleeps.
My son likes to snuggle in my homemade cotton jersey no-sew wrap (instructions here). It makes it easier for him to block out distractions and fall asleep, and then I can put the edge of the cloth over his head so it stays secure while he sleeps.I practiced babywearing a little with my daughter, especially when she got heavier--I would put her in a pouch sling on my hip. Then I had two hands and my arm wouldn't get tired. I also had one of those commercial carriers with the buckles and straps, but it was a low-end one and not very comfortable (it didn't distribute the weight very well to the hips or across the shoulders).
I am glad I decided to do the wrap for my son. I started using it when he was very small (I am wearing him in my blogger profile pic, you can barely see his tiny head--my how he has grown in not yet seven months). A wrap is such a simple way to carry a baby--you just need a long piece of cloth and someone (even if that someone is on youtube) to show you how to tie it.
I am not an avid babywearer or a babywearing expert. I don't babywear everyday. I don't scorn the use of bouncers, jumper-roos, swings, or even strollers. I own all of these things and find them useful sometimes. I use babywearing where it can benefit me, and find it benefits my babies, too.
Babywearing makes having two kids a lot easier, especially when we go out. It is a lot safer to wear my son and put my daughter in the seat of the shopping cart than it is to put my son in the seat of the shopping cart and my daughter in the basket (which is also impractical because I could never trust that little scavenger from opening all the food). It is also nice to wear my son and either push my daughter in a stroller or have my hands free to hold her hands instead of trying to juggle her, the baby, and the diaper bag. And it's great for those times when I really need to cook dinner or clean the kitchen and my baby is tired or fussy and wanting to be held.
When I do babywear, I do so proudly. I welcome all the compliments and questions I get about my wrap, and smile when strangers point it out to their partners and tell them they "want one like that." When other moms who babywear see me with my son in the wrap, I know they recognize me as one of their own. Many babywearers, especially those who use simple, traditional carriers like the wrap, are also part of the natural childbirth movement. I believe that the reason that babywearing and empowered childbirth are linked is because they are both parts of women's wisdom that have traditionally been passed from generation to generation, were lost in the industrial revolution, and now being rediscovered.
When I babywear, I know my baby is safe and happy close to the womb that was his home just a year ago. When I babywear, I treasure it, because I know before long my baby will grow up and never be a baby again, and what better way to savor his babyhood while I still can?
Babywearing has gotten some bad press from the CPSC recently, and baby carriers are being targeted as an "unsafe" product, which they are not. This post was written as part of a campaign to promote baby carriers as the natural, safe, useful tool they are. Please visit the linky at Adventures in Babywearing, and add your own post on why you love/need babywearing and the safety of wearing your baby (and you'll be entered to win a free sling!), and visit the Baby Carrier Industry Alliance page on Facebook, where you can also add links.
Friday, October 1, 2010
Beanies With Love
Wednesday, September 22, 2010
Do I Really Need to be Induced? Resources for Informed Decisions
There are people out there who know what they're talking about more than your student doula/prospective childbirth educator. I've decided instead of writing about this myself, to provide a list of links to various resources available for information on this topic. I have tried to offer multiple perspectives by including links to many types of sources, including research information, statements from professional organizations, care provider opinions, and consumer-oriented information. If you find a link that you feel would be helpful to include in this list, feel free to let me know in the comments.
Suspected Fetal Macrosomia ("The Baby is Too Big")
- Induction of labor for suspected fetal macrosomia (Cochrane Review)
- ACOG Issues Guidelines on Fetal Macrosomia (American Family Physican)
- Big Baby Bull (by Sheridan of Enjoy Birth)
- "is my baby too big?" (Charis Birth Support)
- A Timely Birth by Gail Hart (Midwifery Today)
- The Lie of the EDD: Why Your Due Date Isn't When You Think by Misha Safranski(Associated Content)
- Induction of labor for improving outcomes for women at or beyond term (Cochrane Review)
- Induction of labor: balancing risks--Midwife Thinking's Blog
- Postdates - from Ronnie Falcao's Midwife Archives
- Oligohydramnios: Too Little Amniotic Fluid - March of Dimes
- Birth Sense: Low Amniotic Fluid: A Cause for Panic? (original post has become unavailable, but I found the text reposted on another site)
- Gloria Lemay: Low Amniotic Fluid. . . I don't think so
- Amniotic fluid index versus single deepest pocket as a screening test for preventing adverse pregnancy outcome (Cochrane Review)
- Planned early birth versus expectant management (waiting) for prelabor rupture of membranes at term (Cochrane Review)
- Pre-labor rupture of membranes: impatience and risk--Midwife Thinking's Blog
- Prelabor Rupture of Membranes--PROM--from Ronnie Falcao's Midwife Archives
- High Blood Pressure During Pregnancy - March of Dimes
- Preeclampsia Causes, Symptoms, Diagnosis, and Treatment by eMedicineHealth.com
- Pregnancy-Induced Hypertension - from Ronnie Falco's Midwife Archives
Monday, September 20, 2010
Why Natural Childirth is Not Important
I recently followed an online discussion among student doulas about the use of the term "cesarean birth." Some women wanted cesareans to be recognized as births and some women felt that a cesarean is never a birth because it removes the mother from physically participating in the birth process--since birthing is a verb, and a women having a cesarean is not acting, but being acted upon, it can't be a birth. This lead me to re-examine my definition of what birthing entails.
What does it mean to give birth?
Natural childbirth is not important. A woman being involved in the decisions about the medical care of her and her baby--that is what is important. Helping women avoid feeling assaulted because they were not involved in what happened during their births--that is the goal. What I do--this blog, becoming, a doula and childbirth educator--that is what it is all about.
Thursday, September 16, 2010
the Women in the Scriptures blog is having a giveaway
Monday, September 13, 2010
Marwa's Hypnobabies Birth Story--a must read!
Thursday, September 9, 2010
We are Daughters: my guest post at the Gift of Giving Life
Wednesday, September 8, 2010
Passing knowledge on to the next generation
I've been thinking about how sometimes our choices impact future generations. There has been a lot of talk about circumcision lately, due to reports that the circumcision rate has dropped drastically over the past four years. The vulnerability of circumcised men is one of the reasons that circumcision has been perpetuated from generation to generation in America.
Interestingly, both my husband's and my parents, having children in the '80s when the circumcision rates in the U.S. were somewhere around 80%, broke with this particular tradition. After recently reading an article that discussed how circumcision affects sexuality, I feel that I am lucky that my mother-in-law chose to stick with what was normal in the culture she grew up in, regardless of the culture she was living in at the time. My in-laws' decision made the decision to keep our son intact very easy. The more people stop circumcision in their own families, the faster the custom of non-religious routine infant circumcision will end, since circumcised adult males are some of the biggest propagators of circumcision myths, (for reasons explained in the piece on vulnerability linked above).
I've been thinking about other things mothers can do to benefit future generations. My own mother had a beautiful birth journey. Her first was born by induction for term PROM (sound familiar?) with an epidural and forceps. She had hoped to avoid interventions because she didn't have health insurance, but she was birthing at a hospital and with a doctor both still known for being very medical model (and her doctor was still praciting when I had my daughter in that same town, though I went to a different hospital). Her other three she was able to have less medicalized experiences, using shots of narcotics for two of them and having a drug free birth with her fourth and final birth. Her two youngest were caught by nurse-midwives.
I hope my son (and any brothers that may come along) will understand the importance of supporting his future wife's intuition and helping her find her inner strength in her preparation for the births of their children
"Mothers who have fears also hand down fearful attitudes about birth to daughters--and to every other woman who will listen. But each woman who gains the confidence to birth as unhindered or freely as her biological circumstances will allow--she will go on to encourage her sisters and daughters with birth words and images which resound with all the potential strength and beauty of birth." --Jan Tritten
If not my children, perhaps my grandchildren, will live in a world where fear of birth is not the dominant attitude; a society where the medical world provides support and back-up for the natural process of childbirth; a world where all women are confident in their ability to give birth.
(to learn more about circumcision and intact males, see birthnaturally.org's consumer information on circumcision and peaceful parenting's prepuce and circumcision resources)
Saturday, September 4, 2010
Nursing in Public at the Space Needle

Thursday, September 2, 2010
Did someone say something to you that had an impact on your birth?
Hi Everyone,First of all, just a reminder that Kerry and Carole are speaking at the"Uniting for the Future of Birth" Mega Conference in Milwaukee in early October! http://www.futureofbirthconference.org/ Our session is called, TheTransformative Language of Birth and will allow us to teach birthprofessionals how to alter their thinking and use positive wording which canpositively affect birth outcomes. Please post and e-mail this to EVERYONE!
Since our session at the Mega Conference is all about helping birthprofessionals learn positive language that is extremely helpful to all pregnant and birthing moms, we would like to ask for everyone's input! Thisincludes moms and birth care professionals.Please call our toll-free hotline at 800-350-2204 and complete any or all ofthe following:
"When I was pregnant my (caregiver) said ...to me and then I felt....aboutchildbirth". (Doulas, doctors, midwives, nurses; any caregiver)
"My birth was awesome (or whatever adjective you'd like to use) because my(caregiver) said..."
"My birth was going very well (or however you'd like to describe it) until my (caregiver said ..."
If you are a birth professional, you can complete the following:
"I attended a birth where a (medical caregiver) said....to the birthing momand it changed....in her birth experience (explain what happened, positiveor negative).
Please forward this to anyone who would like t be part of the process ofchanging birth language. Thanks so much for helping us educate birth careprofessionals how to become more positive and effective!
Kerry
Kerry Tuschhoff, HCHI, CHt, CI
I think I have some things I can share. During my son's birth my OB said both some wonderful things and one or two things that could have been said in better ways ("Try not to push" was a big one for me) If you have an experience, whether it was related to a birth with hypnosis or not, they would love to hear from you.
Tuesday, August 31, 2010
Physiological 3rd Stage, without the "as long as..."
If it is true that keeping mother and baby together reduces the risk of hemorrhage, then that is a good reason not to cut the cord immediately. According to Dr. Nicholas Fogelson of AcademicOBGYN,research does not support the current standard practice of immediate clamping. (I also love this post also because of his example of routine episiotomy as a practice that is very obviously passe. I know from a first hand conversation that there are some dinosaur OBs out there who don't stay up to date on research who still use them liberally--I should post about that conversation sometime)
Someone on the Childbirth International e-mail group recently shared a link to a beautiful series of birth photos by Patti Ramos called Emergence. One of the photos shows an attached cord that is simply beautiful. I never knew they were that color.
Later timing of cord clamping may better for both mother and baby. However, after two hospital births where clamping occured earlier than I preferred both times, I have come to believe that physiological cord clamping is still quite rare in hospitals. I think this is partly because they have been conditioned to believe that routine immediate clamping is normal and may subconsiously look for a reason to cut the cord, partly because they have narrow parameters for what constitutes a "healthy" newborn and are quick to provide support, and partly because they aren't set up to provide transitional support to neonates without moving them away from their mothers. Often "delayed" cord clamping is only available at special request and "as long as the baby is doing okay."
In a post at her blog Midwife Thinking, The placenta--essential resuscitation equipment, one homebirth midwife discusses her reasoning for keeping cords intact no matter what and explains how she goes about doing that. She also talks about obstetric pracitces that contribute to the need for babies to be given support. In a response, Navelgazing Midwife shared pictures of the wooden board she brings to births so that she has a hard surface she could use without cutting the cord in case she ever needs to do chest compressions on a baby.
This just goes to show that in some things, both your choice of provider and the equipment aviailable in your chosen birth location can influence what happens in your birth.



